What is Manual Therapy?
- Kathleen Neal

- Apr 8, 2023
- 4 min read
This is the most common question I get as a manual therapist, followed closely by "What made you decide to become a PT?". I can guarantee that each manual therapist you come across will have their own way of treating people, so my answer might not be fully satisfactory. I can, however, describe what I do as a manual therapist and how I have honed my skills over the last near-decade of practicing as a Physical Therapist.

Integrating the Systems
Above, what you see is a relatively creepy picture that divides the major systems of our body. Can you guess two that it neglects to demonstrate here? If you guessed Integumentary System and Female Reproductive Tract, then you win the prize of knowing that you are correct! We are complicated beings and the confusing part is putting all of these together to work as optimally as possible for you.

Need More Information?
Manual Therapists utilize their hands, vision, and intuition to help correct something that has gone wrong in one or more of the above systems. We can see a scar from surgery on the skin, but we feel the depth of the restriction of the scar tissue with our hands and use our intuition to know what other structures can be affected. I see this commonly with C-Section scars, as my focus is on women's health, and I have to determine what else is restricted to improve her symptoms. I'll give you a case study:
35 year old Female 9 months postpartum from cesarean section delivery of healthy baby girl, second child. She is still breastfeeding. Symptoms include chronic low back pain, worsening as baby grows, increased bladder urgency and frequency since delivery, and constipation- going once every 2-3 days. She takes a Vitamin D supplement but no other meds.
What I see: Cesarean section incision scar at lower abdomen, well-healed, left hip slightly higher than the right, right foot more turned out with slightly depressed arch appearance when compared to left.
What I feel: Restriction from all directions from C-Section scar (she did not have any post-op care other than ObGyn saying "it's healed"), mostly from left of scar and below to left hip and pubic bone.
Bringing in my intuition: Because I am an anatomy expert, I know that the incision affects her uterus, the surrounding fascia, and her bladder, which lies behind the pubic bone. The scar tissue does not have elastic properties, so it creates a binding effect to give it as much stability as possible, causing many layers of fascia to bind with it and restricting other areas that require mobility from said fascia. As that pulls, it restricts muscular range of motion, which affects bony alignment of her hips, pubic bone, and sacrum. She is likely carrying her baby on her left hip to use her right hand for writing, opening doors, etc., and has not had any follow up care or PT until now. Given hormone changes not only from immediate post-birth but while she continues to breast feed, her joints maintain a slight laxity. The left side of the incision could also be restricting her sigmoid colon, the last part of the large intestines before diving behind the uterus to become the rectum and then anus.
What I do: My job is to use my manual therapy skills to help release some tension around the scar tissue, improve bony alignment, give gentle exercises and postural awareness to decrease stress on her spine and hips, and educate my patient in how she can help herself at home. The scar is there and can never fully go away, but you can help the structures around it free up and improve their function.
Follow up: Patient returns in 1 week for follow up, states that low back pain is improved and she is more careful with her posture and positioning of the baby, her constipation has improved by 75%, and she is no longer experiencing the bladder urgency and frequency symptoms are improving. Her hips are more level and there is less restriction from the C-section scar, what remains continues to the left abdomen/hip. I continue to work on her right leg and foot posture and review what she is doing at home. I instruct her in a bladder program to schedule her voiding times and to create a bladder diary to see if there are any patterns that arise.
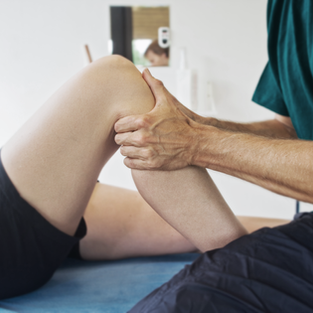
Manual Therapy could look like the following: working on the visceral system, integrating the nervous system by working on the cranium and neck, or a simple joint mobilization of the knee to improve a person's gait following knee surgery.
As a practitioner, there's not one specific thing I do that on repeat for every patient that comes through my door. You are a unique individual and your treatment should be unique as well. In some instances it's a light, constant pressure or a trigger point release, or rolling the fascia and scar tissue mobilization to help free up bound tissue while reeducating the associated muscles.
I often use a two-handed technique to allow one part of the body to communicate with it's associated part on the spine where the higher level nervous system comes into play. For example, I will have one hand on a person's bladder with another hand on the spine level T10-T12 if they have overactive bladder symptoms, bringing awareness to these two areas to allow communication and for my hands to determine if the issue is truly at the bladder or at the spine itself. Considering all of the fascia and muscle attachments in those areas, I then look broader from there. It's a puzzle that we work through together, sometimes with trial and error, but mostly with success.
For my patients with chronic autoimmune issues such as Lyme disease, Hashimoto's, Lupus, and Fibromyalgia, manual therapy helps their nervous system fight their constant battle by bringing them from a constant sympathetic nervous system tone to a more parasympathetic nervous system tone. For those, there is no known cure but definitely a way to help manage it.
Do you have any further questions regarding manual therapy and how it is a helpful part of physical therapy? Send me an email at integralfoundationspt@gmail.com









Comments